Expert Perspectives on Hepatic Encephalopathy
Introduction
Hepatic encephalopathy (HE) is a brain dysfunction caused by liver insufficiency and portal systemic shunt. It manifests as a wide spectrum of neurological or psychiatric abnormalities ranging from subclinical alterations to coma. The “Hepatic Encephalopathy in Chronic Liver Disease: 2014 Practice Guideline by the American Association for the Study of Liver Diseases and the European Association for the Study of the Liver” is a comprehensive guideline on the diagnosis, evaluation, and management of HE (1).
The recommendations put forth in the HE guidelines suggest preferred approaches to the diagnostic, therapeutic and preventive aspects of care and are based on relevant literature and the expertise of the authors (1). However, in healthcare overall, there is a significant implementation gap between the knowledge gained from clinical trials that are put into guidelines versus how clinicians actually practice. Advanced practice practitioners (APPs) who are actively involved in the management and treatment of patients with HE, have provided their expert perspectives on the AASLD/EASL guidelines on HE. In particular, these APPs have identified areas on the guidance that require elaboration. The result is this summary.
Algorithm for the Diagnosis and Management of Overt Hepatic Encephalopathy (1)*
Click on a question for more information.
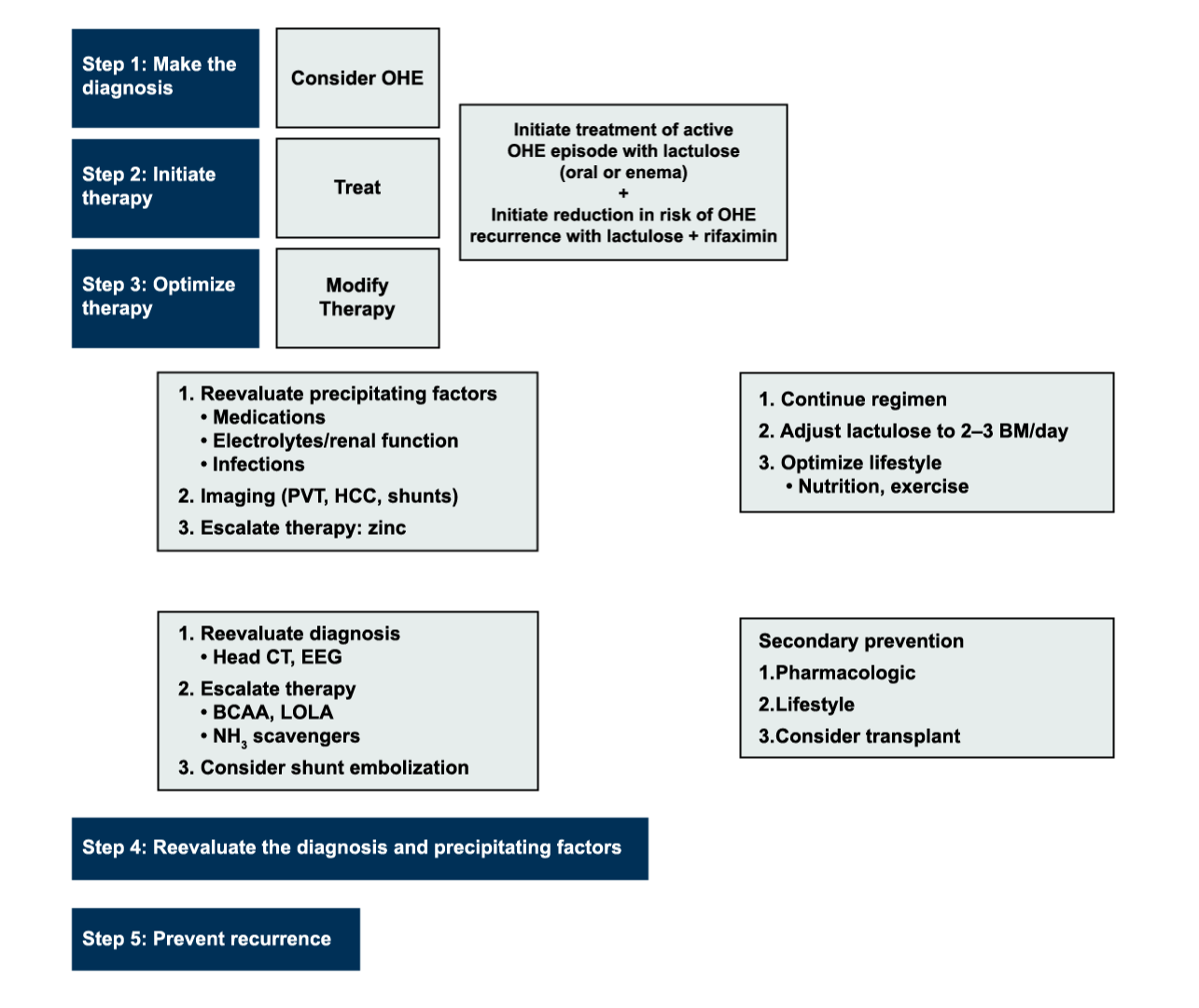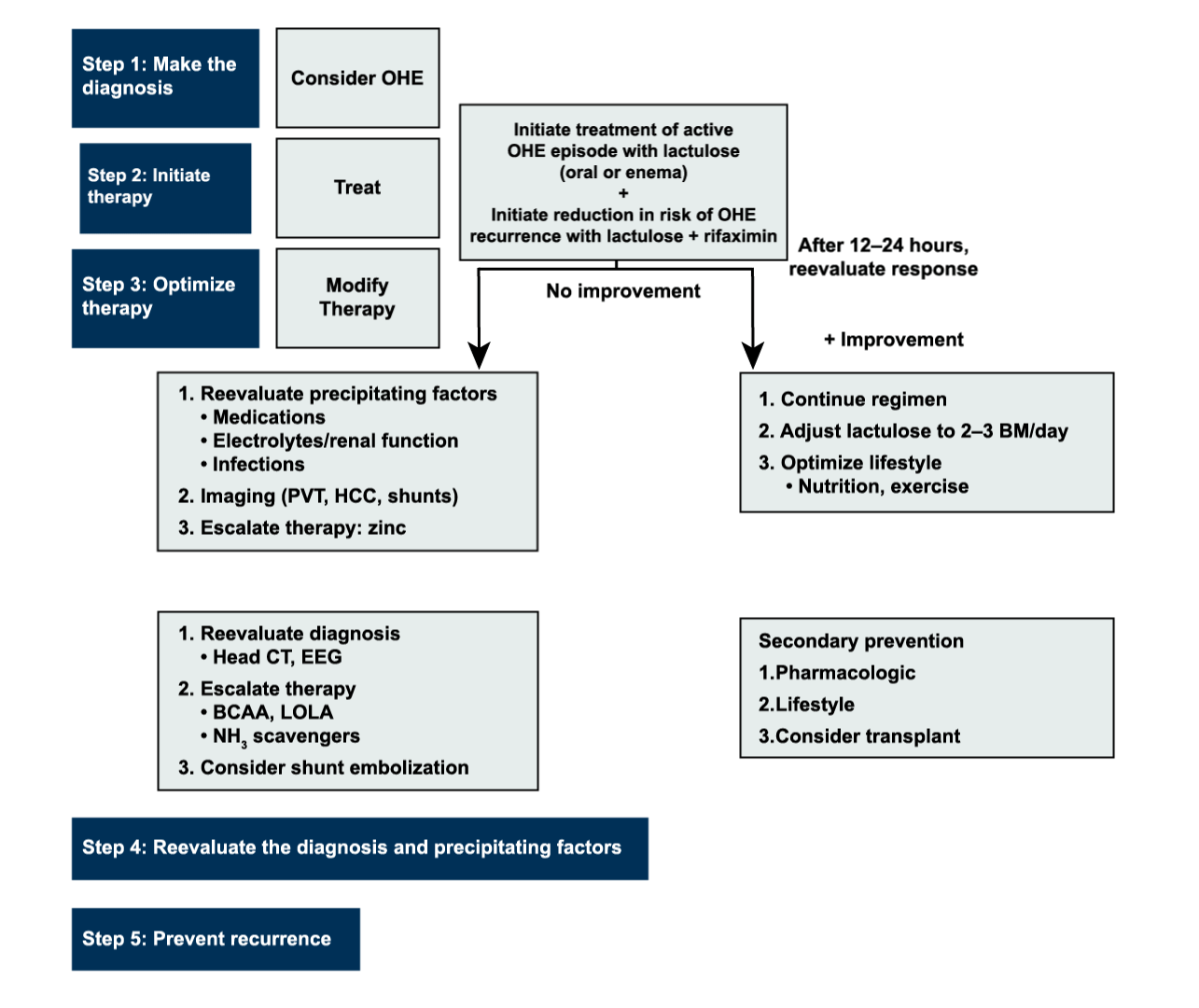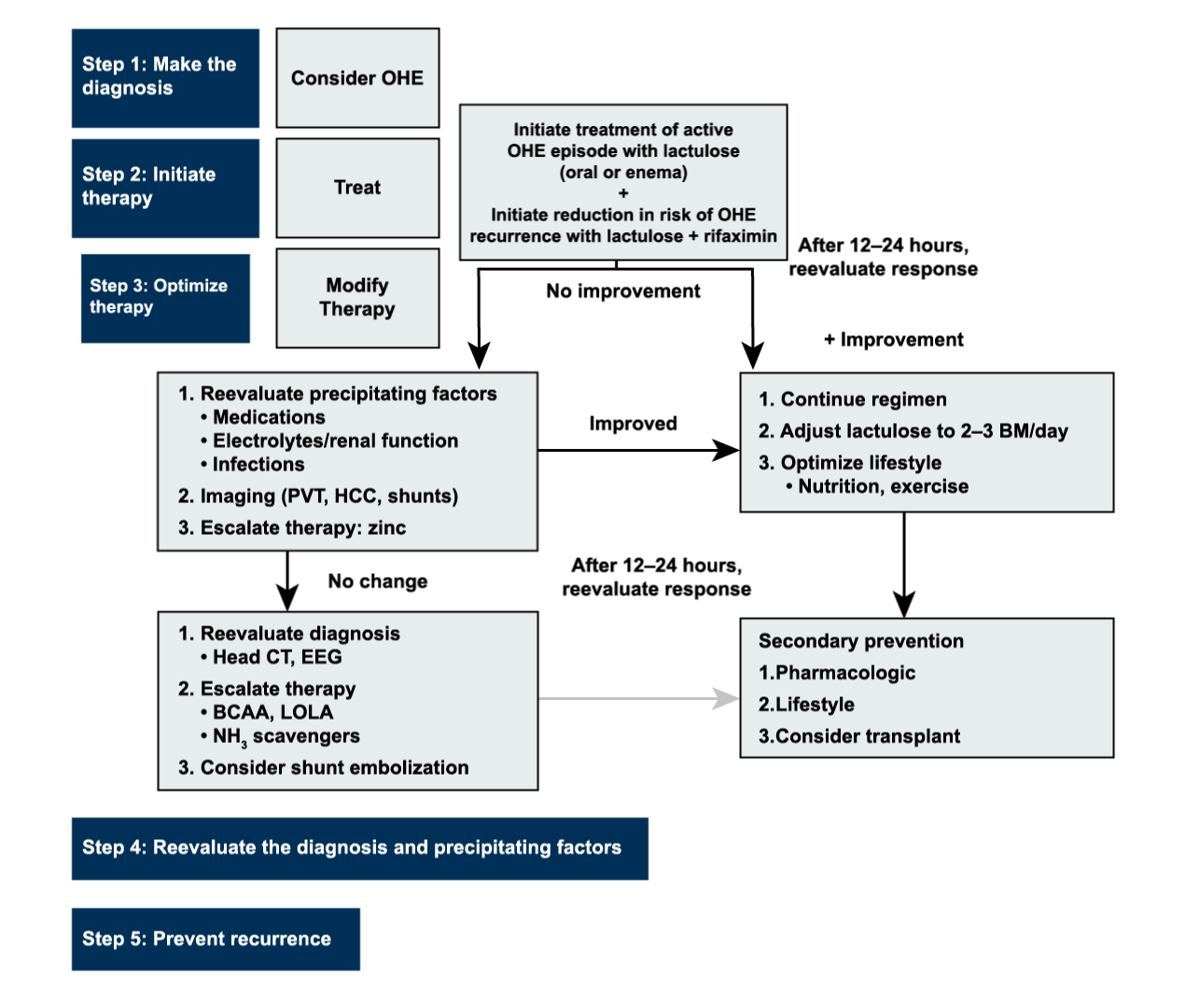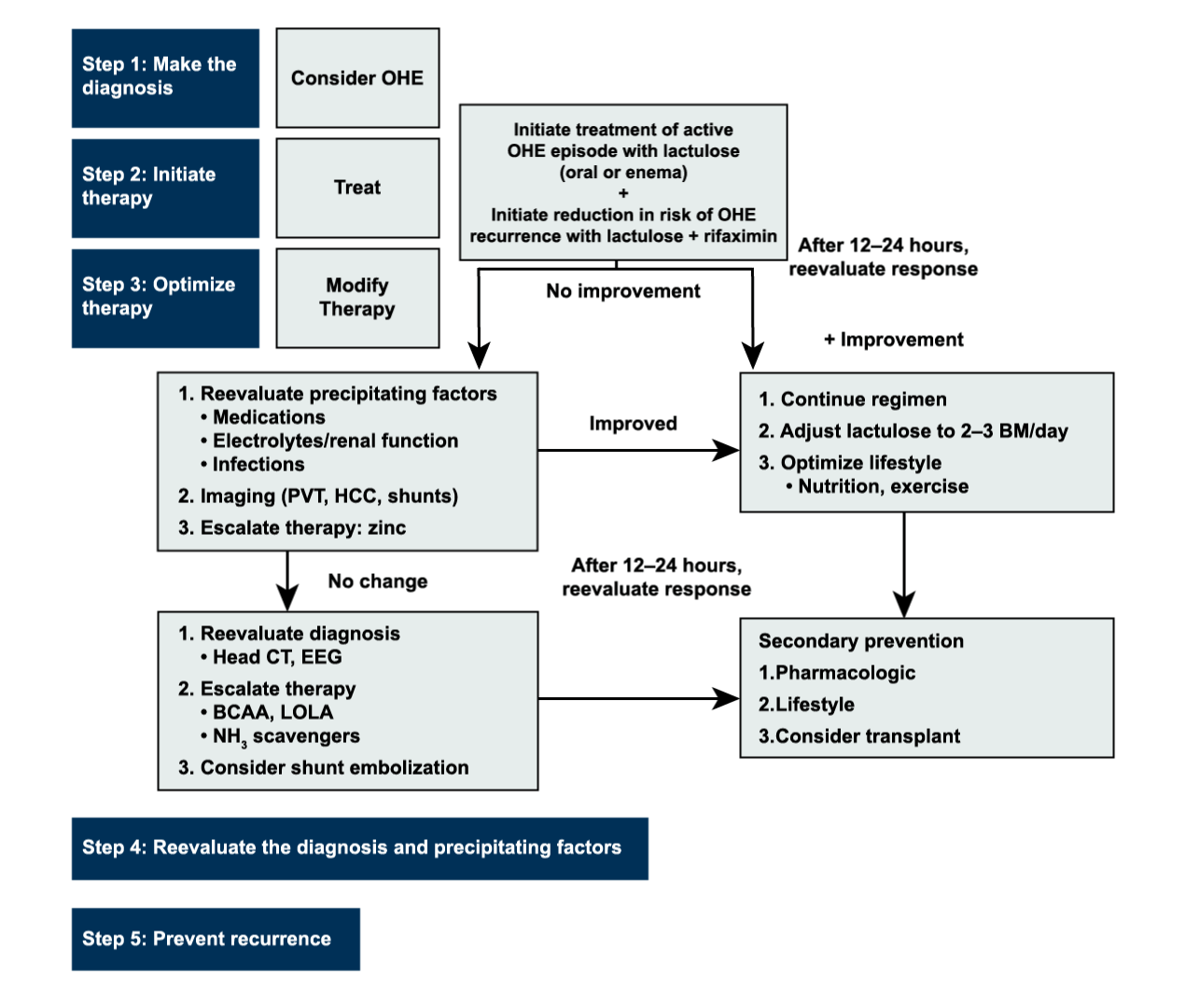
Reau et al. Gastro and Hep. 2016;12(12):S5.
*This algorithm is based on the AASLD/EASL HE Practice Guideline and has been published in the Reau et al. publication. Further recommendations on additional OHE topics (e.g., how to address precipitating factors along with OHE treatment, the role of dehydration in OHE) can be found in the “Hepatic Encephalopathy in Chronic Liver Disease: 2014 Practice Guideline by the American Association for the Study of Liver Diseases and the European Association for the Study of the Liver” publication.1
Click on a topic below for more information.
How do we risk stratify before the first episode of HE?
AASLD guidelines state that “the recognition of precipitating factors for HE (e.g., infection, bleeding, and constipation) supports the diagnosis of HE (1).” However, the guidelines do not address identifying patients at risk for HE before an episode occurs or implementing early intervention prior to the first episode of HE in at-risk patients.
All patients with cirrhosis are at risk of developing HE, irrespective of whether they have experienced a prior episode or not, including those with evidence of malnutrition or frailty and those with evidence of portal hypertension (HTN). Patients experiencing early signs may not be capable identifying HE as they will be in a compromised state. It is recommended that all patients with cirrhosis and their caregivers
be educated on how to recognize early signs and symptoms of HE as part of cirrhosis disease state education. Education encompasses effectively conveying details about the progression of cirrhosis and its related complications (e.g., HE, varices), maintaining awareness of HE symptoms, and emphasizing the significance of mitigating precipitating factors such as constipation. Additionally, it involves addressing other risk factors and triggers associated with HE. Cirrhosis care follow-up visits should involve the provider questioning the patient about any signs of potential HE, including nocturnal sleep disruption and changes in personality and handwriting, impairment in executive function, and difficulties performing activities of daily living. Family support is encouraged in HE, but if a patient brings a family member into the office because they may not be able to retain all of the information on their own, this is potentially suggestive of early HE. Providers should be detailed in their questioning of patients and family members to capture signs and symptoms of HE.
How do we employ the diagnostic tests recommended by the AASLD?
AASLD recommends that the diagnosis of overt (O) HE be based on a clinical examination and a clinical decision. Effective October 2022, K76.82, a billable/specific ICD-10-CM code for HE, became available and can be used to indicate an HE diagnosis for reimbursement purposes. This code is applicable to HE, not otherwise specified, HE without coma, hepatocerebral intoxication, and portal-systemic encephalopathy (2).
AASLD considers the West Haven criteria the gold standard clinical scale for analyzing severity and lists neurophysiological and psychometric tests to aid in this analysis (e.g., Stroop Test, Continuous Reaction Time (CRT) Test, Inhibitory Control Test (ICT)) (1). AASLD recommends that these tests be performed by “experienced examiners” (1). Due to the unpredictable/variable nature of how a patient with potential HE may present on any given day, these tests can also prove to be unreliable and ineffective. Most practitioners do not use these tests in day-to-day practice.
How can compliance and proper diet be encouraged to optimize therapy?
AASLD recommends that all episodes of HE be treated and routine prophylaxis should start after the first episode. Lactulose syrup, 25 mL every 1–2 hours until at least 2 soft or loose bowel movements/day are produced, is the first choice for treatment of an OHE episode. Subsequently, the dosing is titrated to maintain 2–3 bowel movements per day. Secondary prophylaxis after an episode for OHE is recommended (1). Rifaximin, one 550 mg tablet 2 times a day (3), is recommended by AASLD as an effective add-on therapy to lactulose for the prevention of OHE recurrence (1). Rifaximin is the only FDA-approved treatment for the prevention of HE (3).
For optimal effects of therapy, compliance should be assessed and encouraged. It is recommended that a second person regularly observe the patient taking the medication. The most important goal is prevention of recurrent HE episodes. The more that brain injury can be prevented, the better.
Patients often express resistance towards preventive treatments, particularly when it comes to taking rifaximin. Some argue that since they don’t have an infection, they don’t need an antibiotic. It is crucial to address this misconception through proper education. Well-informed patients are generally more compliant with their treatment plans.
Moreover, malnutrition can play a significant role in HE. Therefore, it is important to provide education on protein consumption goals. Additionally, recommendations against unnecessary protein restriction should be addressed, following the appropriate guidelines.
How do we close the revolving door of hospital readmissions?
To prevent rehospitalizations due to HE, AASLD encourages planning outpatient post-discharge consultations. These consultations are essential for adjusting treatment and addressing precipitating factors, aiming to avoid the recurrence of HE episodes. However, this doesn’t always occur due to failure to provide clear patient education in the hospital, delayed patient follow-up, lack of coordination of care, and high drug costs. Some solutions are proposed in the table.

Risk for admission for recurrent HE could decline with education of patients and family members. Examples of important educational messages include the importance of prevention of precipitating factors and how to titrate lactulose when constipation occurs. Patients experiencing an episode of OHE are unreliable, and it could be risky to send them home for self-care, irrespective of the severity of the episode as HE episodes are fluid and symptoms may become worse or better.
References
-
Vilstrup H, Amodio P, Bajaj J, et al. Hepatic encephalopathy in chronic liver disease: 2014 Practice Guideline by the American Association for the Study of Liver Diseases and the European Association for the Study of the Liver. Hepatology 2014;60:715-35.
-
2023 ICD-10-CM Diagnosis Code K76.82 Hepatic Encephalopathy. Available at: https://www.icd10data.com/ICD10CM/Codes/K00-K95/K70-K77/K76-/K76.82#:~:text=2023%20ICD%2D10%2DCM%20Diagnosis,82%3A%20Hepatic%20encephalopathy. Accessed August 17, 2023.
-
Xifanan [Package Insert], Bridgewater, NJ: Salix Pharmaceuticals, Inc. 2022.
This Expert Perspective on Hepatic Encephalopathy was supported by Salix Pharmaceuticals.
